People with severe, untreated obstructive sleep apnea are nearly three times more likely to die from cardiovascular causes than those without the condition.
And yet, an estimated 80 to 90 percent of sleep apnea cases go undiagnosed. Most people have no idea their nightly breathing pauses are doing that kind of damage.
Sleep apnea has no obvious signs of sleep apnea you can see while awake — no chest pain, no visible warning. It works quietly, night after night, straining your heart, spiking your blood pressure, and starving your brain of oxygen while you sleep.
If you’ve been told you may have sleep apnea or already have a diagnosis, here’s what leaving it untreated actually costs you.
Understanding Sleep Apnea and Why It Matters
Sleep apnea is a condition where breathing repeatedly stops and starts during sleep. These pauses can last from a few seconds to over a minute and may happen hundreds of times a night.
The three main types are obstructive sleep apnea (OSA), in which the throat muscles relax and block the airway; central sleep apnea (CSA), in which the brain fails to send proper signals to the breathing muscles; and complex sleep apnea syndrome, a combination of both that sometimes occurs after OSA treatment begins.
OSA is the most common, affecting an estimated 1 billion people worldwide. Regardless of type, untreated sleep apnea puts steady pressure on the heart, lungs, and brain over time, quietly raising the risk of serious, life-limiting health conditions.
Who is Most at Risk for Sleep Apnea?
Sleep apnea can affect anyone, but certain factors significantly increase the risk of developing this condition.
Risk Factors:
- Obesity: Excess tissue narrows the airway.
- Neck circumference: Larger than 17 inches (men) or 16 inches (women) signals a higher risk.
- Male sex: Men are twice as likely, though the gap narrows after menopause.
- Age 40+: Muscle tone declines, increasing airway collapse.
- Menopause: Hormonal changes increase risk, with symptoms often misdiagnosed.
- Alcohol/sedatives: Relax throat muscles, worsening apnea.
- Smoking: Narrows the airway.
- Family history: Genetics play a role in airway structure.
- Nasal issues: A small jaw or large tonsils can restrict airflow.
Understanding these risk factors can help identify potential sleep apnea cases, leading to early diagnosis and effective treatment.
Sleep Apnea and Your Lifespan: What You Need to Know Untreated sleep apnea can significantly reduce life expectancy due to the increased risk of heart disease, stroke, high blood pressure, and other complications. On average, severe untreated sleep apnea may shorten life expectancy by up to 7–8 years, second only to lifelong cigarette smoking. However, with proper treatment, such as CPAP therapy, many individuals can manage the condition and significantly reduce these health risks. |
How Untreated Sleep Apnea Reduces Life Expectancy
Can you die from sleep apnea? Most people underestimate how dangerous the condition can actually become. Not usually in a single night, but that doesn’t mean the condition is harmless.
The real danger is cumulative. Each night of disrupted breathing adds more strain to the systems your body depends on to stay alive long-term.
Research consistently links untreated sleep apnea to shorter life expectancy through several overlapping pathways:
- Chronically elevated blood pressure, even during the day
- Increased sleep apnea, stroke risk, and heart attack risk
- Worsening insulin resistance raises the risk of type 2 diabetes
- Persistent inflammation that damages blood vessel walls over time
People with severe, untreated sleep apnea are significantly more likely to die from cardiovascular disease than those who receive treatment or don’t have the condition at all.
According to the National Library of Medicine, the longer it goes untreated, the greater the damage to vital organs.
Health Risks Associated with Untreated Sleep Apnea
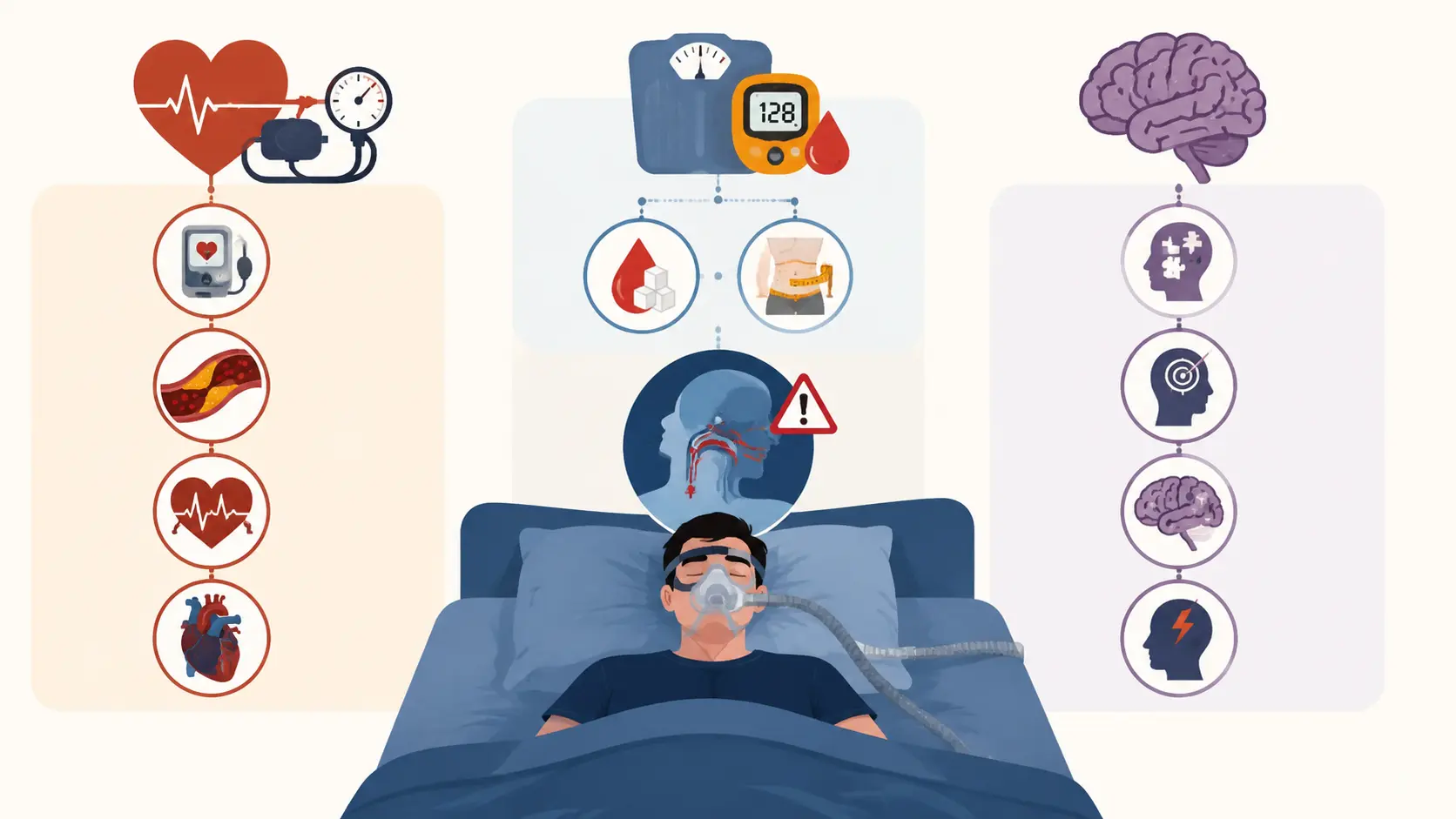

Cardiovascular Risks
When breathing stops during sleep, the body triggers a stress response. Heart rate jumps. Blood vessels tighten.
Blood pressure, a direct consequence of the sleep apnea–blood pressure feedback loop, repeatedly spikes throughout the night.
Over years of nightly repetition, this wears down the cardiovascular system in ways that don’t reverse on their own.
The condition has claimed several well-known figures whose deaths brought renewed attention to how quietly fatal untreated sleep apnea can be.
People with untreated sleep apnea face an increased risk of:
- High blood pressure (hypertension), including cases resistant to medication
- Coronary artery disease and heart attack
- Atrial fibrillation, an irregular heart rhythm that raises stroke risk
- Heart failure
Studies show that people with untreated obstructive sleep apnea are two to three times more likely to experience a heart attack compared to people without sleep-disordered breathing.
Metabolic Risks
Disrupted sleep directly affects the hormones that regulate blood sugar and appetite. People with untreated sleep apnea are more likely to develop type 2 diabetes, even when controlling for body weight and other lifestyle factors.
The condition also promotes weight gain, particularly around the abdomen, worsening the severity of sleep apnea.
Neurological and Cognitive Risks
Repeated drops in blood oxygen affect the brain over time. People with untreated sleep apnea frequently experience memory problems, difficulty concentrating, and slower reaction times.
Long-term, the condition raises the risk of stroke and has been linked to earlier onset of cognitive decline and dementia in some studies.
The Biological Effects of Untreated Sleep Apnea on the Body
When sleep apnea goes untreated, it disrupts more than just rest. The repeated lack of oxygen and the chronic activation of your stress response can damage vital organs, accelerating aging and increasing the risk of serious conditions.
Oxygen Deprivation
Every apnea episode drops blood oxygen levels. The body responds by jolting the sleeper just enough to restart breathing, which rarely produces full consciousness but does prevent the deep, restorative sleep stages the body needs.
Night after night, this cycle of oxygen drops and micro-arousals keeps the body under constant low-grade physiological stress.
Over the years, repeated oxygen deprivation damages the lining of blood vessels, increases cellular oxidative stress, and accelerates aging in the heart, kidneys, and brain.
Sympathetic Nervous System Activation
Untreated sleep apnea chronically triggers the body’s “fight or flight” response. Stress hormones like cortisol and adrenaline stay elevated not just during sleep, but throughout the day.
Sustained activation of the sympathetic nervous system contributes to high blood pressure, chronic inflammation, and metabolic disruption, all of which reduce life expectancy when left unaddressed.
Mental Health Implications of Untreated Sleep Apnea
Can sleep apnea cause anxiety? Research strongly suggests it can, and the relationship between the two conditions runs deeper than mere tiredness.
When sleep is fractured night after night, the brain’s ability to regulate emotion and stress breaks down. People with untreated sleep apnea report higher rates of:
- Generalized anxiety disorder
- Depression
- Irritability and mood instability
- Difficulty managing stress
The connection isn’t one-directional. Poor sleep worsens anxiety, and anxiety raises physiological arousal at night, making quality sleep harder to achieve. This cycle keeps both conditions in place.
The good news: treating sleep apnea often produces measurable improvements in mood and anxiety levels, sometimes within weeks, without any additional mental health intervention.
Understanding the Impact of Sleep Apnea Severity on Life Expectancy
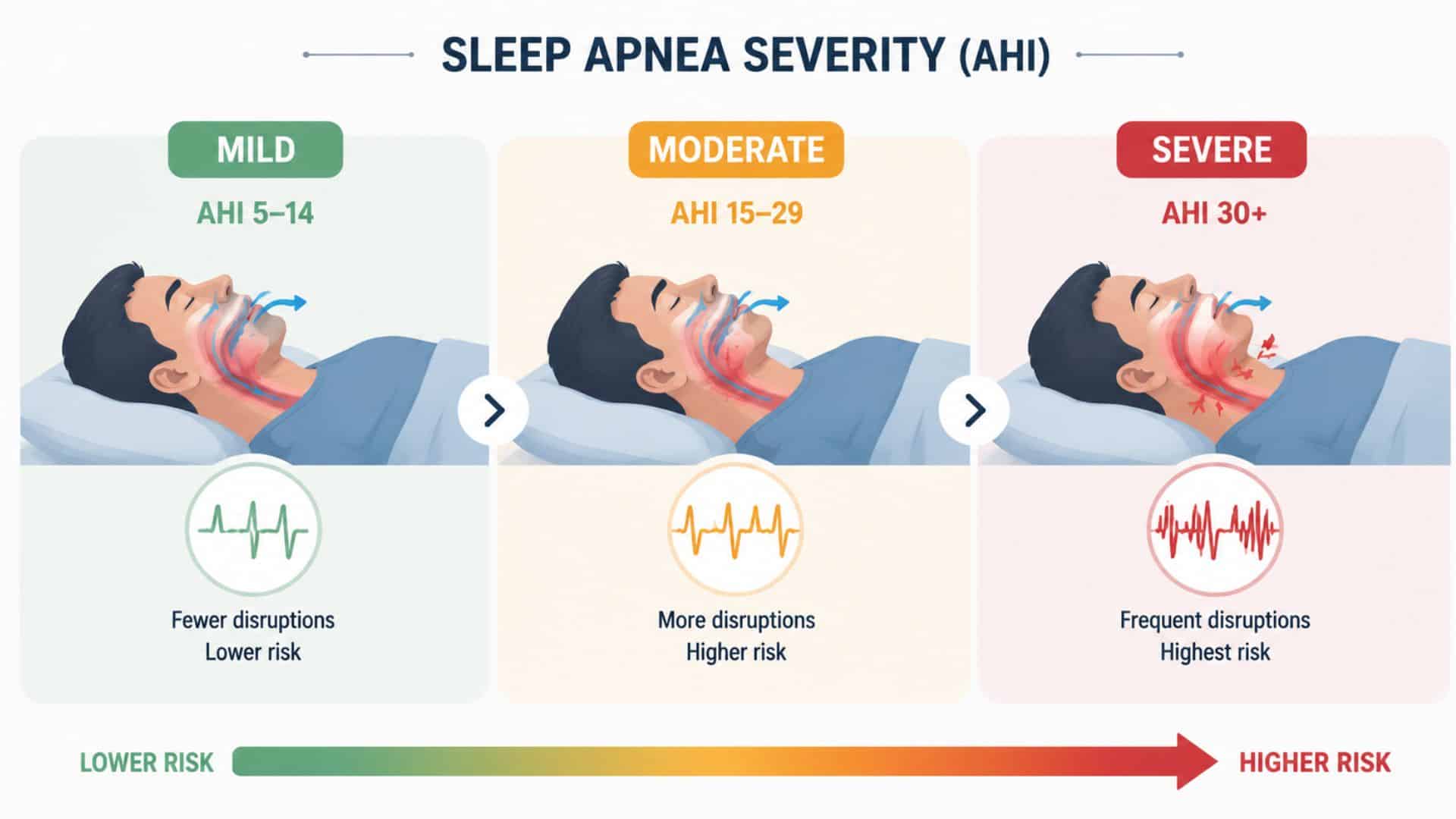

Sleep apnea severity determines which obstructive sleep apnea treatment options are recommended, and it’s measured using the apnea-hypopnea index (AHI), which counts breathing disruptions per hour of sleep.
- Mild (AHI 5–14): Breathing disruptions are less frequent. Health risks are present but lower. Mild sleep apnea often worsens over time, particularly with age or weight gain, if not addressed.
- Moderate (AHI 15–29): Cardiovascular strain, daytime fatigue, and cognitive effects become more pronounced. Risk of serious long-term health complications increases significantly at this level.
- Severe (AHI 30+): The highest-risk category. Severe, untreated sleep apnea is associated with a substantially higher likelihood of early death from heart disease, stroke, and related conditions.
Even mild sleep apnea warrants attention. Without treatment, the condition rarely stays mild.
The Role of Treatment in Extending Life Expectancy
Treating sleep apnea can reverse many of its effects and meaningfully reduce the risks tied to untreated sleep apnea. The right obstructive sleep apnea treatment options depend on the type and severity of the condition. Here’s how the main choices compare:
CPAP Therapy
The benefits of CPAP therapy extend well beyond better sleep. Consistent CPAP use has been shown to lower blood pressure, reduce cardiovascular risk, and improve cognitive function in people with moderate to severe OSA.
BiPAP Therapy
Bilevel positive airway pressure (BiPAP) delivers different pressure levels for inhaling and exhaling. It’s typically used for central sleep apnea or for patients who find CPAP uncomfortable or difficult to tolerate at higher pressures.
Oral Appliances
Custom-fitted oral appliances reposition the jaw to keep the airway open during sleep. They’re a practical option for people with mild to moderate obstructive sleep apnea, particularly those who struggle with CPAP adherence.
Lifestyle Modifications
Weight loss, reducing alcohol consumption, avoiding sedatives before bed, and sleeping on your side can all reduce the severity of sleep apnea. These changes work best as a complement to medical treatment, not a replacement for it.
Case Studies: How Treatment Can Improve Your Life Expectancy
The real-world data backs up what clinical research shows.
An analysis of long-term CPAP users found that their rates of cardiovascular events dropped to levels comparable to those of people without sleep apnea at all.
In documented case series, patients with severe obstructive sleep apnea who started consistent CPAP therapy saw meaningful reductions in daytime blood pressure, with the largest gains seen in people with resistant hypertension, where reductions of around 10 mmHg have been documented, substantially enough to lower stroke risk.
Patients who received treatment also reported major improvements in energy, mental clarity, mood, and quality of life. Many described the shift as dramatic rather than gradual.
The pattern across the literature is consistent: people who treat sleep apnea live longer and healthier lives than those who don’t, regardless of which treatment method they use.
Summing Up: How Early Diagnosis Can Extend Your Life Expectancy
Untreated sleep apnea isn’t just a sleeping problem. It’s a slow-moving cardiovascular, metabolic, neurological, and mental health risk that compounds over time.
The connection between untreated sleep apnea and life expectancy is well-established, and the damage builds quietly for years before most people know it’s happening.
Early diagnosis gives you the best shot at avoiding that compounding harm.
At-home sleep tests are now widely available and have been validated against in-lab polysomnography, making getting diagnosed easier, faster, and less expensive than ever before. Most are covered by major insurance plans with a physician referral.
If you snore loudly, wake up gasping, feel exhausted after a full night of sleep, or struggle with unexplained anxiety or high blood pressure, bring it up with your doctor.
The sooner sleep apnea is caught and treated, the better your odds of a longer, healthier life.
Frequently Asked Questions
Can You Have Sleep Apnea Without Snoring?
Yes, up to 25% of people with sleep apnea don’t snore. Gasping, morning headaches, and persistent daytime fatigue can also point to the condition.
How is Sleep Apnea Diagnosed?
A sleep study, done in a clinic or at home with a portable monitor, measures breathing patterns, oxygen levels, and sleep disruptions overnight.
Does Sleep Apnea Get Worse With Age?
It often does. Throat muscle tone naturally decreases with age, increasing the likelihood of airway collapse during sleep and making apnea episodes more frequent over time.











