Sleep paralysis can feel scary. You wake up but cannot move or speak, and it may feel very real. Many people face this at least once. So, what is sleep paralysis, and what causes it?
It often happens when your body and mind are not in sync during sleep. Poor sleep, stress, and certain habits can trigger it.
If you want to know how to prevent sleep paralysis, simple daily changes can help. Small steps like better sleep habits and a calm bedtime routine can lower the chances and help you feel more in control at night.
What is Sleep Paralysis?
Sleep paralysis is a type of parasomnia, a sleep disorder that causes unusual experiences just before, during, or after sleep. It is directly connected to REM sleep, the stage where most dreaming occurs.
During REM sleep, your brain temporarily stops your muscles from moving. This is called REM atonia, and it prevents you from physically acting out your dreams.
Sleep paralysis occurs when your mind wakes up, but the muscle paralysis has not yet lifted. It can happen while falling asleep or waking up, and episodes last a few seconds to several minutes before ending on their own.
According to Sleep Medicine Reviews, around 7.6% of the general population experiences it at least once, most commonly starting during the teenage years or early adulthood.
Why Sleep Paralysis Happens During REM Sleep?
Your body moves through sleep in cycles of about 90 minutes, and each cycle includes REM sleep, where most dreams happen.
During this stage, your brain is very active, but it also relaxes your muscles to stop you from acting out your dreams. Sleep paralysis happens when this timing gets mixed up.
Your mind wakes up and becomes aware, but your body is still in this relaxed state.
This creates a short gap where you cannot move or speak. REM sleep periods become longer in the early morning, which is why episodes often happen then.
The part of the brain linked to fear stays active, making the experience feel intense.
Signs and Symptoms of Sleep Paralysis


Sleep paralysis can feel different for everyone, but certain symptoms show up again and again. Here is what most people experience during an episode.
1. Physical Symptoms
These are the most noticeable signs that happen to your body during an episode:
- You cannot move your arms, legs, or any part of your body
- You cannot speak or call out for help
- You feel a heavy pressure on your chest, as if something is sitting on top of you
- Breathing may feel more difficult than normal
- You can still move your eyes and breathe on your own throughout the episode
2. Hallucinations
Along with physical symptoms, many people also experience hallucinations. According to the Sleep Foundation, these occur in roughly 75% of sleep paralysis episodes and are very different from regular dreams. There are three common types:
- Sensing or seeing a threatening presence or dark figure in the room
- Feeling intense chest pressure or the sensation of being physically held down
- Feeling like you are floating, flying, or leaving your own body
3. Emotional Symptoms
Once the physical symptoms set in, strong emotions tend to follow:
- Intense fear or panic during the episode
- Feeling confused or shaken once the episode ends
- Anxiety or dread about falling back to sleep afterward
- Long-term worry about going to bed, which can affect overall sleep quality
Knowing these symptoms makes it easier to understand what is happening in the moment. Recognizing them is the first step toward learning how to prevent sleep paralysis from disrupting your nights.
What Causes Sleep Paralysis?
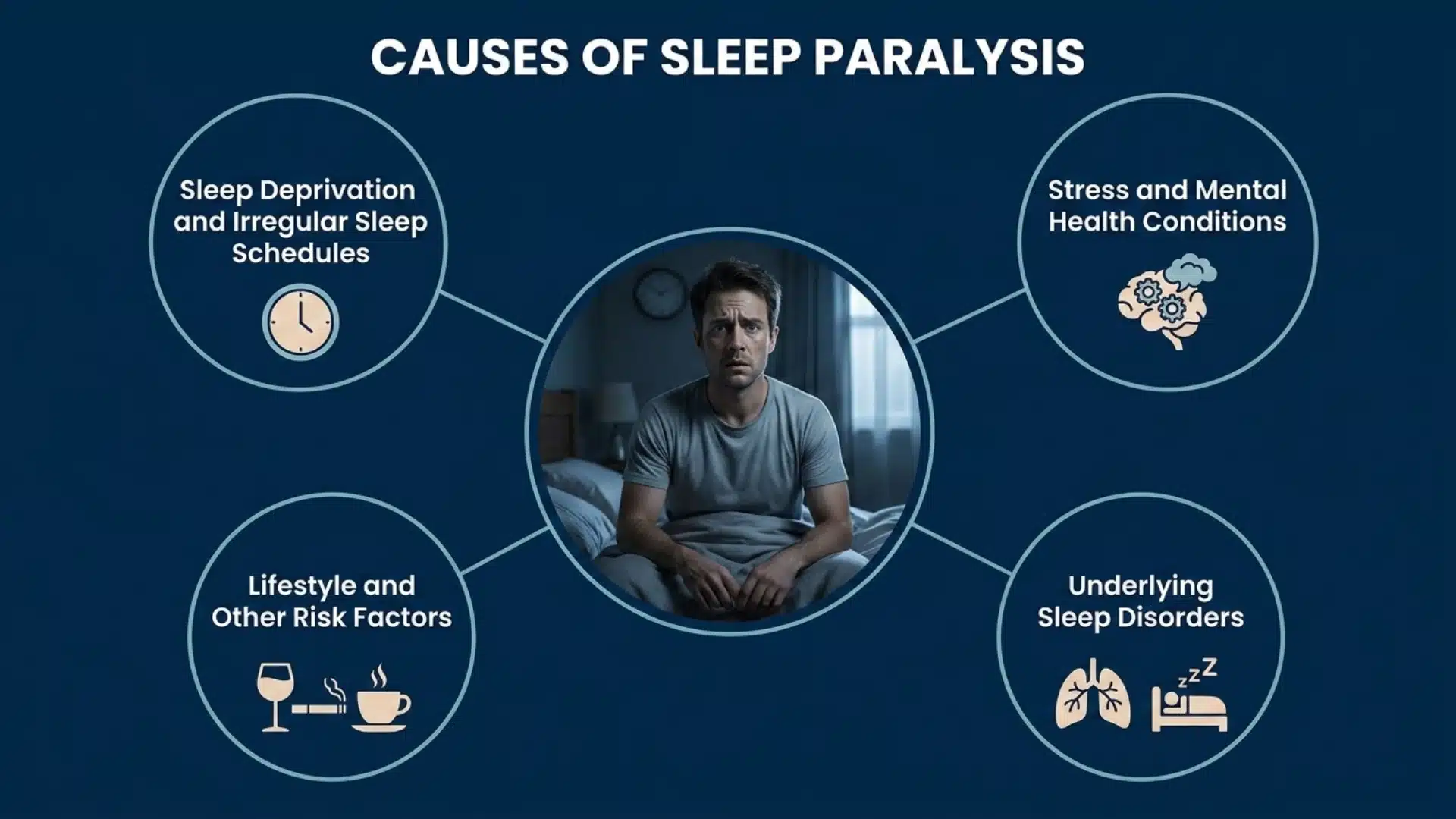

Sleep paralysis does not always happen randomly. Several habits and health conditions increase the likelihood. Knowing your triggers is the first step toward better sleep.
- Sleep Deprivation and Irregular Sleep Schedules: Your body needs steady, consistent sleep to move through sleep stages properly. Without it, REM sleep hits too fast and disrupts the process.
- Stress and Mental Health Conditions: A brain that stays on high alert at night has trouble fully switching off. People with PTSD, panic disorder, and bipolar disorder face a higher risk.
- Underlying Sleep Disorders: Conditions like narcolepsy and obstructive sleep apnea affect how your brain controls sleep. These disorders make the shift between sleep stages unstable and harder to manage.
- Lifestyle and Other Risk Factors: Certain daily habits and personal factors can quietly raise your risk over time. Sleeping on your back, some ADHD medications, and even family history all play a role.
Everyone’s triggers are different. Once you spot what’s affecting your sleep, it becomes much easier to take the right steps and reduce future episodes.
How to Prevent Sleep Paralysis?
Sleep paralysis can feel scary, but simple daily habits and a solid sleep hygiene checklist can help you stop it from happening again.
1. Maintain a Consistent Sleep Schedule
Going to bed and waking up at the same time every day helps regulate your body’s internal clock. When your sleep cycle becomes stable, REM sleep transitions run more smoothly.
This lowers the risk of a timing mismatch between your brain and body, which is a key trigger for episodes.
2. Get Enough Quality Sleep (7 to 9 Hours)
Sleep deprivation is one of the strongest triggers of sleep paralysis. When your body is overtired, it enters REM sleep too quickly.
This abrupt shift increases the chance of disruption between wakefulness and REM atonia. Aiming for 7 to 9 hours each night gives your body enough time to cycle through sleep stages properly.
3. Sleep on Your Side Instead of Your Back
Sleeping flat on your back has been strongly linked to more frequent sleep paralysis episodes. Side sleeping helps reduce airway pressure and supports more stable REM transitions.
If you tend to roll onto your back at night, placing a pillow behind you can help. Side sleeping is also a better position for people dealing with lower back pain, making it a smart switch for more than one reason.
4. Reduce Stress and Mental Overload Before Bed
High stress keeps your brain partially alert during sleep, raising the chance of mixed sleep states. A simple calming routine before bed can help your brain shift into rest mode.
Try deep breathing, light stretching, or writing down your thoughts. You can also follow simple sleep habits like the 10-3-2-1-0 rule to create a consistent wind-down routine and improve overall sleep quality.
5. Limit Caffeine and Alcohol in the Evening
Caffeine delays sleep onset, and alcohol disrupts REM cycles later in the night. Both fragment your sleep pattern and increase the chance of REM instability.
Cutting off caffeine by early afternoon and avoiding alcohol close to bedtime gives your body a better chance of moving through sleep stages without interruption.
6. Improve Your Sleep Environment
A dark, quiet, and cool room helps your body stay in deeper sleep stages throughout the night. Poor sleep conditions increase the frequency of brief awakenings, which increases the risk of REM disruption.
Simple changes like blackout curtains, a white noise machine, or lowering the thermostat can make a noticeable difference.
Small changes to your sleep routine can make a big difference. Start with one tip tonight and build from there.
What to Do During a Sleep Paralysis Episode?
During a sleep paralysis episode, the best thing you can do is stay calm and remind yourself that it will pass.
It may feel scary, but it is not harmful and usually ends within a minute or two. Try to focus on slow, steady breathing to help your body relax.
Instead of struggling, gently try moving a small part of your body, such as a finger, toe, or even your tongue, as these may respond first.
Avoid forcing large movements, as this can increase fear. Keeping your eyes closed or shifting your focus can also help. Repeating a simple thought like “this will pass” can make the experience feel less intense.
When to See a Doctor?
Sleep paralysis is usually not dangerous, but you should talk to a doctor if it happens often or starts affecting your daily life.
If episodes occur more than once or twice a month without a clear cause, they may require medical attention. Feeling strong fear at bedtime or being very sleepy during the day are also warning signs.
Sudden muscle weakness during the day, especially with strong emotions, should not be ignored.
Very vivid hallucinations that continue after waking can also be a concern. If simple lifestyle changes do not help after a few weeks, a doctor may check for sleep disorders or related mental health conditions.
Conclusion
Sleep paralysis is unsettling, but it does not have to control your nights. Once you understand what causes sleep paralysis and what triggers it in your body, stopping it becomes much easier.
Small changes like adjusting your sleep schedule, changing your sleeping position, and reducing stress before bed can make a real difference.
If episodes keep happening, talking to a doctor is always a smart step. Start with one change tonight. Your brain and body both deserve rest that feels safe, calm, and uninterrupted every single night.
Frequently AskedQuestions
Can Sleep Paralysis Be Cured Permanently?
There is no permanent cure, but consistent sleep habits, stress management, and treatment of underlying conditions can significantly reduce episodes over time.
Is Sleep Paralysis More Common in Certain Age Groups?
It most commonly starts between ages 14 and 25, with teenagers and young adults reporting the most episodes.
Can Sleep Paralysis Run in Families?
Yes, research suggests a possible genetic link, meaning if a close family member experiences it, your risk may be higher too.











