Waking up tired every single day is exhausting. And doing it while wearing a mask attached to a loud machine? Even more so.
CPAP is effective; no one’s arguing that. But it isn’t easy to live with. The noise, the straps, the dry mouth, the feeling of being trapped. Millions of people give up on it every year, and honestly? That’s understandable.
What most people don’t realize is that CPAP isn’t the only option.
Figuring out how to sleep with sleep apnea without CPAP is more achievable than most people assume.
There are many doctor-recognized alternatives, from simple lifestyle adjustments to advanced medical treatments, and one of them may be right for your specific situation
Sleep apnea is serious. But finding a treatment that fits your real life is completely within reach.
What is Sleep Apnea and Why Does It Need to Be Treated?
Sleep apnea is more than loud snoring. It’s a serious sleep disorder where your breathing repeatedly pauses during sleep, sometimes hundreds of times a night.
The most common type, obstructive sleep apnea (OSA), occurs when soft tissue in the throat relaxes and blocks the airway, even in people who have never snored.
Central sleep apnea (CSA) is less common and happens when the brain doesn’t send the right signals to the breathing muscles.
Most of the CPAP alternatives in this article are for OSA, so CSA should always be managed by a specialist.
Untreated sleep apnea can leave you tired, foggy, and irritable. Over time, it may also raise your risk of high blood pressure, heart rhythm problems, stroke, and depression.
Sleep apnea severity is measured by AHI, or breathing disruptions per hour:
| Severity | AHI Score | Common Options |
|---|---|---|
| Mild | 5–14 | Positional therapy, oral appliances, lifestyle changes |
| Moderate | 15–29 | Oral appliances, BiPAP/APAP, Inspire, surgery |
| Severe | 30+ | Inspire, MMA surgery, BiPAP, GLP-1 if weight is a factor |
Your AHI score helps your doctor match the treatment to your actual risk. Skipping treatment isn’t safe, but switching to one that fits your life can be.
Struggling With CPAP

Alt Text: Person struggling with a CPAP mask showing discomfort and sleep apnea frustration
CPAP is clinically proven and widely considered the gold standard for treating sleep apnea, but that doesn’t mean it works for everyone in practice.
A significant number of people prescribed CPAP struggle with consistent use, and the reasons are very real: the mask feels claustrophobic, the constant airflow is uncomfortable, the machine hums through the night, and the tubing makes it hard to move around in bed.
For frequent travelers, it adds another layer of hassle. Some users wake up with dry mouth, skin irritation, or pressure sores from the mask straps.
The important thing to understand is that sleep apnea treatment isn’t one-size-fits-all. What works perfectly for one person may feel completely unbearable for another.
The goal isn’t to force yourself through a treatment you can’t tolerate; it’s to find one you’ll actually stick with.
13 Ways to Sleep With Sleep Apnea Without a CPAP Machine
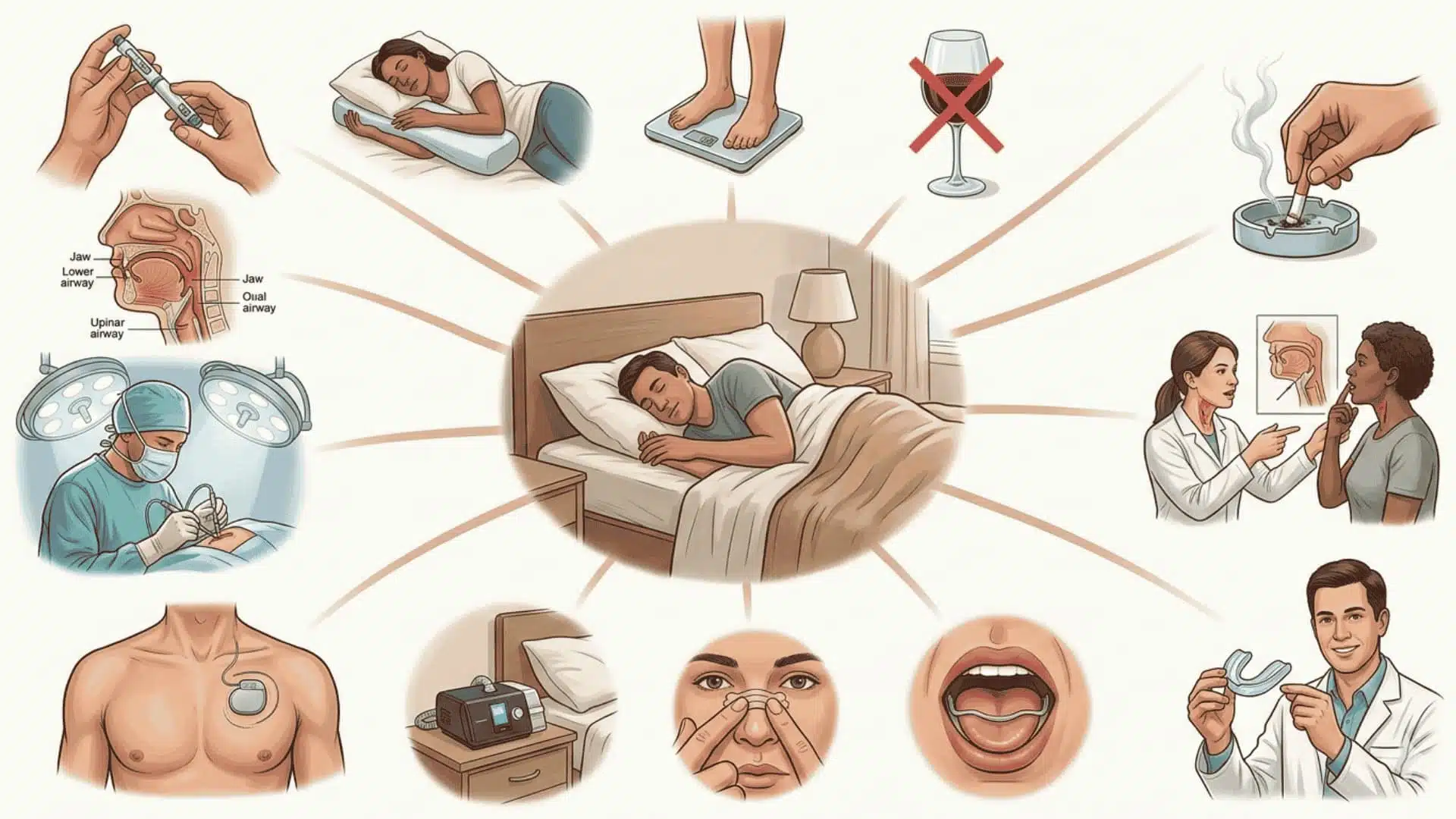
Alt Text: Realistic illustration showing 13 sleep apnea treatment alternatives to CPAP surrounding a peaceful sleep scene
Not ready for a CPAP machine, or just done trying to make it work? Here are 13 clinically recognized alternatives, ranging from simple daily changes to advanced medical options, so you can find what fits your life.
1. Positional Therapy
For many people, sleep apnea is significantly worse when lying flat on their back. In this position, gravity pulls the soft tissues of the throat downward, narrowing or fully blocking the airway.
Simply switching to side sleeping can noticeably reduce apnea episodes. Specially designed positional pillows, anti-snore vests, or even the old tennis-ball-in-the-pajamas trick can help train your body to stay off its back through the night.
2. Weight Loss
Carrying excess weight, especially around the neck and throat, puts added pressure on your airway during sleep. It’s one of the strongest risk factors for obstructive sleep apnea.
There is also atwo-way relationship between sleep apnea and body weight, where poor sleep may make weight harder to manage, while excess weight can worsen airway blockage.
Research shows that weight loss can reduce sleep apnea severity by reducing the number of breathing interruptions at night. Even modest weight loss can lead to noticeable improvements.
In some cases, weight loss directly reduces fat around the airway, including the tongue. A study supported by the U.S. National Heart, Lung, and Blood Institute (NHLBI) found that reductions in tongue fat were a key factor in the improvement of sleep apnea after weight loss.
For people with mild to moderate OSA, this can significantly improve symptoms and, in some cases, even resolve the condition altogether.
3. Avoid Alcohol and Sedatives Before Bed
Alcohol and sedative medications relax the muscles throughout your body, including those responsible for keeping your throat open during sleep. Even one or two drinks close to bedtime can cause the soft tissue at the back of your throat to droop into the airway, significantly worsening apnea.
A practical rule of thumb is to avoid alcohol at least three to four hours before sleeping and to speak with your doctor if you rely on sleep medications.
4. Quit Smoking
Smoking can irritate and inflame the upper airway, making the breathing passage narrower during sleep. This may worsen obstructive sleep apnea by increasing the likelihood of airway collapse.
Research published through the National Library of Medicine notes that smoking may affect OSA through upper-airway inflammation, sleep quality changes, and altered breathing control. Another meta-analysis found that secondhand smoke exposure may also be linked with a higher risk of OSA.
Quitting smoking may help reduce airway irritation over time and support better breathing during sleep. It may not cure sleep apnea on its own, but it can be a strong step in managing OSA.
5. Myofunctional Therapy
Think of this as physical therapy for your throat. Myofunctional therapy uses targeted tongue, throat, and facial exercises to strengthen the muscles that help keep your airway open during sleep.
These exercises may help reduce OSA severity, especially in mild cases. They also fit well with other natural approaches to improving airway health, though they work best when guided by a trained provider.
Newer devices, such as eXciteOSA, use gentle electrical stimulation during the day to help strengthen airway muscles without wearing a device at night.
6. Oral Appliance Therapy
Oral appliances, often called mandibular advancement devices, are custom-fitted mouthguards made by a specialized dentist. They work by gently pushing the lower jaw and tongue forward, keeping the airway open throughout the night.
Over 100 FDA-approved designs exist, and they are silent, portable, and require no power, making them ideal for travelers. They are most effective for mild to moderate sleep apnea and are the most commonly prescribed non-CPAP treatment available.
7. Tongue Retaining Devices
Unlike mandibular advancement devices that reposition the jaw, tongue-retaining devices hold the tongue forward using gentle suction, preventing it from falling back and blocking the airway. These are particularly useful for patients who cannot wear jaw-repositioning appliances due to dental issues, missing teeth, or jaw pain.
Custom-fitted versions from a dentist tend to be more effective than over-the-counter options and should be evaluated alongside your overall treatment plan.
8. Nasal Dilators and Nasal Valve Therapy
Sometimes the problem begins at the nose. Nasal dilators, either internal inserts or external adhesive strips worn across the bridge of the nose, help keep nasal passages open, reducing airway resistance before it even reaches the throat.
For a more clinical option, Provent Therapy uses FDA-cleared nasal valves that create back-pressure on exhalation to maintain airway openness. These are lightweight, travel-friendly, and work best for mild OSA with a significant nasal congestion component.
9. BiPAP and APAP
If your issue with CPAP is specifically the pressure rather than the mask itself, BiPAP and APAP machines offer meaningful relief. BiPAP uses two pressure levels: higher on inhalation, lower on exhalation, making it far more comfortable to breathe against.
APAP automatically adjusts pressure throughout the night based on your real-time breathing needs. Neither is CPAP-free, but both are significantly easier to tolerate and are worth exploring before ruling out PAP therapy altogether.
10. Inspire Therapy
Inspire is an FDA-approved device surgically implanted in the chest that works by stimulating the hypoglossal nerve, the nerve that controls tongue movement. It senses your breathing patterns throughout the night and delivers gentle electrical pulses to keep the tongue and airway muscles engaged, preventing collapse.
There is no mask, no machine, and no noise. Patients activate it with a small remote before bed. It is highly effective for moderate-to-severe OSA in patients who meet specific eligibility criteria.
11. Soft Tissue Surgery
When oversized tonsils, a floppy soft palate, or excess throat tissue are the root cause of your sleep apnea, surgical removal can directly address the problem.
Common procedures include uvulopalatopharyngoplasty (UPPP), which removes excess tissue from the throat and upper palate, and somnoplasty, which uses radiofrequency energy to reduce tissue with minimal recovery time.
In some patients, surgery resolves sleep apnea entirely. In others, it makes other treatments, such as oral appliances, significantly more effective.
12. Maxillomandibular Advancement
MMA surgery physically moves both the upper and lower jaws forward, permanently enlarging the airway. It is one of the most structurally effective surgical treatments for OSA, with strong long-term success rates even in severe cases.
Genioglossus advancement, a related procedure, repositions the attachment of the genioglossus muscle to prevent nighttime collapse. Recovery takes longer than soft tissue surgery, but for patients whose jaw anatomy is contributing to their sleep apnea, MMA can offer results that no device or lifestyle change can match.
13. GLP-1 Medications
Zepbound (tirzepatide) is now FDA-approved to treat moderate-to-severe obstructive sleep apnea in adults with obesity, along with a reduced-calorie diet and increased physical activity. It is the first FDA-approved medication for OSA.
It works mainly by supporting significant weight loss, which can reduce airway blockage during sleep. In clinical studies, people taking Zepbound had fewer breathing interruptions at night compared with those taking a placebo.
This option is not for every sleep apnea patient, especially when airway structure, jaw position, or other causes are involved. A doctor can help decide whether it fits your case.
For those looking to manage sleep apnea at home without a machine, this represents a newer option that may support broader treatment plans under medical supervision.
A note from Lena: Always check with your doctor first Before swapping or stopping any treatment, always loop in your doctor. What works for someone else may not be right for your specific type or severity of sleep apnea. The alternatives on this list are clinically recognized, but they are not interchangeable; your AHI score, anatomy, and overall health all shape which path is appropriate for you. |
Choosing the Right Sleep Apnea Treatment Without CPAP
With many options available, the right choice depends entirely on your specific situation, your severity, anatomy, lifestyle, and the level of intervention you’re comfortable with.
- Apnea Severity (AHI Score): Mild OSA often responds to lifestyle changes and oral appliances. Moderate-to-severe cases typically need stronger device-based or surgical solutions.
- Your Anatomy: Enlarged tonsils, a small jaw, or a large tongue point toward different treatments. An ENT can identify structural contributors that lifestyle changes alone won’t fix.
- Your Lifestyle: Travel frequently? Oral appliances and nasal devices outperform any device that requires a power outlet. Is weight a factor? Addressing it first amplifies the effectiveness of every other treatment.
- Dental Health: Oral appliances require a healthy jaw and a full set of teeth. TMJ issues or missing teeth may rule this option out entirely.
- Tolerance for Procedures: Some people want the least invasive path. Others are open to surgery for a permanent fix. Knowing your comfort level helps your doctor narrow the shortlist fast.
The most important first step is a proper sleep study. A sleep specialist or ENT can match the right treatment to the actual cause, not just the symptoms.
Can You Combine These Treatments for Better Results?
Absolutely, and in many cases, combining approaches is exactly what specialists recommend. Sleep apnea is rarely caused by just one thing, so relying on a single treatment doesn’t always get you all the way there.
Positional therapy paired with an oral appliance, for instance, often outperforms either one used alone. Weight loss combined with myofunctional therapy yields compounding benefits: less tissue pressing on the airway and stronger muscles holding it open.
Even surgery, which doesn’t always eliminate apnea on its own, can make oral appliances or other devices far more effective afterward. Simple lifestyle changes like cutting alcohol, quitting smoking, and side sleeping act as a strong foundation that amplifies whatever clinical treatment sits on top.
Think of it less like choosing one solution and more like building a personal protocol. Start with the easiest changes, layer in stronger options as needed, and stay consistent every night.
Wrap Up
Sleep apnea is serious, but struggling with a CPAP machine doesn’t have to be your only story. From something as simple as changing your sleep position to advanced options like Inspire therapy or GLP-1 medications, the right one is out there for you; it just takes finding it.
Start small, speak to a specialist, and don’t settle for sleepless nights because one treatment didn’t fit.
Because here’s the real question worth sitting with: if there are this many alternatives available, what’s been stopping you from exploring them?
If this blog helped you see your options more clearly, save this page, share it with someone who’s been battling their CPAP, and drop a comment below. We’d love to hear what’s worked for you.
Frequently Asked Questions
Is There a Way to Cure Sleep Apnea without CPAP?
In some cases, yes. Significant weight loss, jaw surgery, or nerve stimulation therapy can resolve sleep apnea entirely, but results vary based on severity and individual anatomy.
What is the 3% Rule for Sleep Apnea?
The 3% rule is a scoring criterion in sleep studies: a breathing event is counted only if oxygen levels drop by 3% or more during the pause.
What is the Average Age of Death for Sleep Apnea?
Untreated sleep apnea has been linked to a higher risk of serious health conditions like heart disease, stroke, and metabolic disorders, which can impact overall life expectancy over time.